Blood glucose meter
How to improve your diabetes therapy
What are blood glucose meters used for?
Self-monitoring of blood glucose is crucial for adjusting insulin doses. For this purpose people rely on an easy-to-use blood glucose meter that can deliver a reliable result quickly.
Blood glucose values refer to the sugar content (glucose level) in the blood, which can change depending on meals and physical activity. The amount of glucose dissolved in the blood is measured and the results are given in „Milligrams per decilitre" (mg/dl) or „Millimoles per litre" (mmol/l).
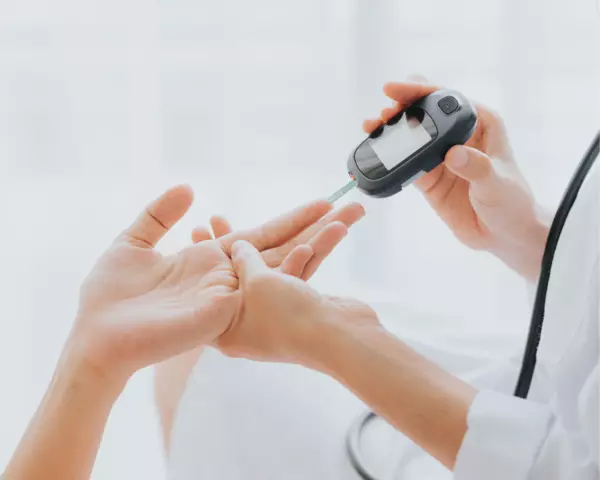
How does the classic capillary blood measurement work?
A capillary blood measurement provides point‑accurate values and is the best known method of measuring blood glucose that a person with diabetes can also perform themselves: you prick the fingertip with a lancet device, obtain a drop of blood, apply it to a test strip inserted into a meter and get the result after a few seconds.
One disadvantage of this method is that it only provides individual readings, meaning blood glucose fluctuations in between remain undetected. In addition, incorrect handling can affect the results and frequent blood glucose testing can be painful and inconvenient.
What are the pros and cons of CGM and FGM systems?
Besides this classic measurement method, there are new monitoring systems that can measure glucose continuously without puncturing blood vessels. These systems allow better control of glucose trends and are known as “Continuous Glucose Monitoring” (CGM).
A thin sensor filament a few millimetres long is usually inserted and adhered to the upper arm and measures the sugar content in the subcutaneous tissue roughly every five minutes. A new sensor typically needs to be applied every six to ten days. Such a glucose monitoring system has a transmitter that sends the values to a receiver (often a smartphone), where the glucose trend can be observed. One advantage of CGM is that lower and upper glucose thresholds can be set individually. As soon as these thresholds are exceeded, an alert sounds. This helps to adjust therapy more effectively.
The “Flash Glucose Monitoring” (FGM) works similarly to a CGM system. However, here you need to hold a scanner (or your phone) up to the sensor to view the current glucose values. Scanning also works through thicker clothing. The sensor is changed every two weeks.
This system is particularly practical for people with diabetes who need to measure glucose values several times a day to manage their insulin therapy themselves. In both systems (CGM and FGM) the sensor can be worn while bathing, showering and swimming and briefly in a sauna.
What are the specifics of long‑term CGM?
There is also long‑term CGM. In this system the sensor is inserted under the skin of the upper arm by a trained physician. The sensor capsule remains under the skin for 180 days. A transmitter is placed on the skin and forwards the measured glucose values to a receiver (usually a smartphone).
If blood glucose falls or rises too much, the transmitter vibrates and the smartphone also gives a warning signal. The transmitter can be removed intermittently, which is advantageous for people who want to stay longer in the water or in the sauna, or who do not tolerate the adhesive well.
Blood glucose under control: best tips for correct home measurement
- As simple and obvious as it may sound: read the user manual before first use of your blood glucose meter and familiarise yourself with your device.
- Wash your hands thoroughly with a mild soap or cleanser before measurement and dry them with a towel. Residues of cream or sugar (for example from fruit) or moisture can distort the results. Make sure your soap does not contain ingredients such as honey or caramel.
- Just before the blood draw you can gently massage or shake your hand to promote circulation. You should wipe away the first drop of blood, as it may contain tissue fluid that can dilute the sample and distort the value. For this reason you should also avoid strong squeezing of the finger, otherwise cell fluid will escape. Hold the test strip to the drop until enough blood is absorbed.
- The lancet must only be used once for blood collection to avoid the risk of infection. Rotate puncture sites and prick slightly to the side of the fingertip where there are fewer pain receptors and more blood vessels. The middle, ring or little finger are best suited for blood collection.
- After measurement, hands should be treated with a moisturising hand cream to care for the stressed skin and prevent infections, since impaired wound healing is characteristic of diabetes mellitus.
- Keep a blood glucose diary. Documented values help to adjust your therapy. You can keep a written diabetes diary, or use blood glucose apps for smartphones. Glucose meters generally store values automatically.
- Never store test strips loose; always keep them in their original container where they are protected from moisture and dirt. Do not use strips that have fallen on the floor. Check the expiry date. All this helps ensure the strips do not give false readings.
- Since blood glucose meters are temperature sensitive, measurement errors can occur below 4 °C and above 30 °C. In extreme cold, for example on a ski holiday, carry your device and strips in an inside pocket. In extreme heat keep them in a cool room. If you store your test kit in a refrigerator, wait before measuring until it has returned to room temperature.
- Note that some medications can distort the result. This includes the painkiller acetylsalicylic acid (if more than one gram is taken one to two hours before measurement).
- The sensor of the glucose meter can generally be applied to the same body sites suitable for insulin injection: abdomen, buttocks, thigh and the back of the upper arm. Refer to the user manual for more precise measurement instructions.
- Never place the sensor on scar tissue. Also bear in mind that readings can be affected by belt buckles, piercings and seat belts.
- Because sensors are waterproof, you can swim, bathe and shower without removing them. However, the adhesive may come loose in the water. It is therefore advisable to secure the sensor additionally with a waterproof plaster.
- CGM receivers are generally not waterproof. If necessary, you can take them along if the receiver is protected by a waterproof pouch. Be aware that the transmitter's radio waves transmit only limitedly in water, which can cause recording disturbances.
- CGM devices measure glucose in the subcutaneous tissue and not in the blood. It should be noted that this value can lag the current blood glucose by about 10 minutes. This should be considered when measuring after meals or exercise, where rapid changes in blood glucose can occur.
- Every 3 to 6 months the CGM meter should be compared with a laboratory device at the specialist practice to check its accuracy.
Anyone can master blood glucose measurement to get a better overview of their glucose values. Blood glucose meters provide more safety in everyday life!