Breast cancer
How early detection saves lives
editorial.overview
What affects the risk of developing breast cancer?
The risk of developing breast cancer is influenced by a variety of factors and the disease does not arise from a single cause. Here are some of the most important influencing factors.
The likelihood of developing breast cancer increases with age. From age 30 onwards the risk steadily rises and up to 80% of breast cancer cases occur after the age of 50.
Tumour cells in breast tissue respond to hormones such as oestrogens and progestogens. The risk is greater the longer the exposure to these hormones. Women whose first menstrual period occurred before age 11 and those who enter menopause after age 54 are particularly at risk.
Women who have not had children have an increased risk of breast cancer. This is because after childbirth a hormonal stimulus causes the milk gland cells to take on their milk-producing function. Without this stimulation, the probability that cells will become malignant is higher. Pregnancies and prolonged breastfeeding, on the other hand, reduce the risk of breast cancer.
Breast cancer can also occur more frequently in certain families, which may be due to genetic factors. Women are at particularly high risk if at least two female first-degree relatives (mother or sister) have had breast and/or ovarian cancer, or if a first-degree relative developed breast cancer before age 50. This also applies if a male family member has had breast cancer. It is important to know, however, that only 5 to 10 out of 100 breast cancer cases are hereditary.
Breast cancer is therefore a complex disease influenced by a combination of genetic, hormonal and environmental factors. Age, hormonal status, childlessness and genetic predisposition are some of the main risk factors. A better understanding of these factors enables women to make informed decisions about screening and prevention.
How do the stages of breast cancer differ?
Staging in breast cancer is crucial for treatment choice and prognosis. The International Union Against Cancer (UICC) distinguishes four main stages based on factors such as tumour size, lymph node involvement and the presence of metastases. Here is a detailed overview of how breast cancer stages differ.
Stage 0 is also called ductal carcinoma in situ (DCIS). It is an early form of breast cancer in which tumour cells are confined to the milk ducts or lobules and have not invaded surrounding tissue. No lymph nodes are involved and there are no distant metastases. The tumour is localised and is often detected by routine mammography before symptoms appear. Chances of cure are very good because the cancer has not spread to other parts of the body.
A tumour in Stage I measures up to 2 cm in diameter. There is no lymph node involvement and no metastases. Chances of cure are high and treatment often consists of a combination of surgery, radiotherapy and, where appropriate, hormone therapy or chemotherapy.
Stage II breast cancer may involve a larger tumour or have already spread to nearby lymph nodes. The tumour measures between 2 and 5 cm or there is involvement of the axillary lymph nodes. There are no distant metastases yet. Treatment can be more complex and often includes surgery, chemotherapy, radiotherapy and hormone therapy. The chances of cure remain good, especially if lymph node involvement is limited.
Stage III breast cancer is more advanced and may have spread to surrounding tissues and multiple lymph nodes. The tumour is larger than 5 cm or has spread to nearby lymph nodes and/or breast tissue. No distant metastases are present. Treatment is more intensive and may combine chemotherapy, surgery, radiotherapy and possibly hormone therapy. Prognosis depends on the exact extent and response to treatment.
Stage IV refers to advanced breast cancer with metastases in other organs such as the lungs, liver or brain. The tumour can be of any size and distant metastases are detectable. The disease has spread to other parts of the body. Treatment aims to control the disease and improve quality of life. Therapy may include chemotherapy, hormone therapy, targeted therapy or a combination of these approaches. Prognosis varies widely depending on response to treatment and extent of metastases.
Tumour grade (grading) assesses how aggressive the tumour is, based on the appearance of tumour cells under the microscope. Some tumours depend on hormones such as oestrogen or progesterone, which can influence treatment options.
Can mammography protect against breast cancer?
Mammography does not prevent the development of breast cancer, but it can make a decisive contribution to early detection. Regular mammography screening can detect small, non-palpable tumours, which significantly increases the chances of successful treatment. Early detection often allows for less invasive treatment, frequently breast-conserving and without extensive surgery or chemotherapy.
Mammography uses X-rays to image the breast in multiple planes and reveal even the smallest changes. About 90% of breast cancer cases can be detected in this way. In women with particularly dense breast tissue or in cases of unclear findings, mammography is often supplemented by additional examinations such as ultrasound (mammasonography) or magnetic resonance imaging (MRI). These complementary methods improve differentiation between benign cysts and potentially malignant tumours.
If breast cancer is suspected, a tissue sample (biopsy) is taken under image guidance and analysed in the laboratory to establish a definitive diagnosis. In this way mammography makes a crucial contribution to early detection and treatment of breast cancer, but it cannot prevent the disease from occurring in the first place.
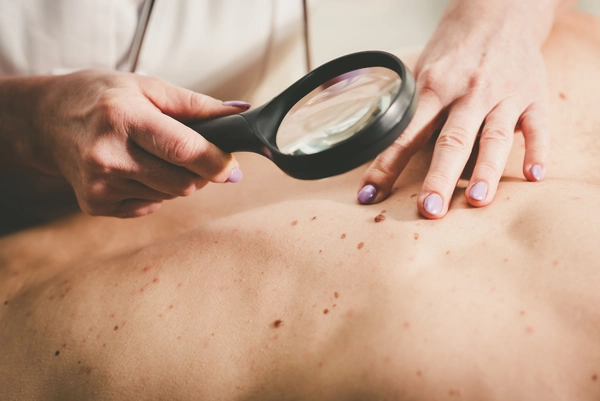
What does the breast look like when someone has breast cancer?
Breast cancer can present in different ways, particularly in the external appearance and texture of the breast. In early stages there are often no symptoms, which is why regular examinations are especially important. If changes occur, they should be examined promptly by a doctor.
Visible and palpable signs include lumps or hardening, changes in size and shape as well as nipple and skin changes. A lump or hardening in the breast or under the arm that is unexplained and does not resolve can be a sign of breast cancer. Unilateral discharge or a retracted nipple can also indicate breast cancer. A noticeable change in breast size or shape, such as swelling or dimpling, should also be investigated by a doctor. Discolouration such as redness or other skin changes can also be a sign of breast cancer.
If you notice these signs, it is important to have them checked by a doctor, as early diagnosis and treatment offer the best chances of cure.
Can I detect breast cancer by self-examining my breasts?
Self-examinations can be helpful in noticing tissue changes that may indicate breast cancer. They are an important part of breast health and can help detect unusual hardening or other abnormalities early. However, self-examinations should not be used as the sole method of early detection.
Mammography is an essential complementary screening tool because it can detect signs of breast cancer before they become palpable. The combination of regular mammography and self-examination offers the best chance of detecting and treating breast cancer early.
Breast cancer diagnosis: what examinations are necessary?
If breast cancer is suspected, several examinations are required to make an accurate diagnosis. The process begins with a detailed medical history, during which the doctor asks about your symptoms and medical background. This is followed by a physical examination, during which the doctor palpates your breasts, checks for swollen lymph nodes and examines the armpits and the clavicle area. This examination can be uncomfortable but is usually painless.
Mammography is a central examination in which the breast is placed between two plexiglass plates and X-rayed to visualise changes in breast tissue. This examination may be uncomfortable but is brief. In addition to detecting tumours, mammography can also reveal microcalcifications that may indicate a precancerous condition.
An ultrasound complements mammography by showing tissue changes using sound waves. This examination is painless and radiation-free and allows assessment of both tumours and swollen lymph nodes.
If cancer is suspected, a biopsy is performed in which tissue samples are taken with a hollow needle. These samples are examined by a pathologist for cancer cells. The tissue sampling is done under local anaesthesia and post-procedure pain is generally mild.
In some cases a magnetic resonance imaging (MRI) is also performed. This exam produces detailed breast images using magnetic fields. MRI can help determine the exact extent of the tumour and provide further information.
Through these diagnostic procedures doctors can reliably determine whether breast cancer is present and how advanced it is, in order to plan the appropriate treatment.
Breast cancer diagnosis: does the breast have to be amputated?
If a mammary carcinoma is detected, there are several treatment options available, including radiotherapy directed at the affected tissue and, in some cases, mastectomy, which involves removing the entire breast.
Whether breast removal is necessary depends on various factors and is decided individually for each patient. In many cases today a breast-conserving operation (BCO) can be performed. This decision is based on factors such as the size and location of the tumour and the patient's overall health. Your treating physician will advise and inform you comprehensively to choose the best treatment option for you.
When is chemotherapy appropriate for breast cancer?
Chemotherapy is appropriate for breast cancer when the aim is to inhibit the growth and multiplication of cancer cells and to shrink or eliminate the tumour. This treatment is usually carried out using cytostatic agents that aim to stop cancer cell growth.
Chemotherapy can be used in two ways: as neoadjuvant therapy to shrink the tumour before surgery, or as adjuvant therapy to kill any remaining cancer cells after surgery. It is an important treatment option particularly for HER2-negative breast cancer or triple-negative breast cancer (TNBC).
During chemotherapy the drugs are usually administered as infusions and can also affect healthy cells in the body. The decision whether and when chemotherapy is appropriate is made in consultation with your treating physician, who considers the individual situation and the specific tumour profile. The risk of recurrence after treatment of a mammary carcinoma can be reduced by careful follow-up and targeted therapies aimed at the tumour's specific receptors.
How to properly feel the breast – how does it work?
- Choose the right time: Perform the self-examination between the sixth and the twelfth day of your cycle, as your breast tissue is less tender and less swollen at this time. For women after menopause a fixed day is recommended, e.g. the 1st of each month.
- Pick a set day each month: Always do your self-exam on the same day of the cycle or month to better notice any changes. You will have a better basis for comparison if you examine your breasts at the same time each month.
- Examine your breast in front of a mirror: Start with an inspection in front of a mirror. Place your hands on your hips, raise your arms and lean slightly forward. Look for differences in size, shape, skin condition and any dimpling or irregularities.
- Feel while standing and lying down: The palpation should be done both standing and lying down. Standing allows easier access to the top and bottom of the breast, while lying down helps distribute the tissue evenly.
- Use circular motions: Use your fingertips to palpate the breast tissue with gentle circular motions. Stand upright and place your hand on the upper outer part of the breast. Then use several fingers and circular motions to move inward toward the nipple.
- Vary the pressure: Change the pressure of your fingers to feel both superficial and deeper tissue layers. Pay attention to any textures or hard areas in the breast tissue.
- Check the armpit area: Statistically, many carcinomas are observed in the armpit area. Also palpate this region thoroughly, as lumps or enlarged lymph nodes often occur here.
- Examine the areola: Press gently on the nipple to check for any discharge or blood. This can be a sign that should be medically evaluated.
- Use aids when needed: Self-examination can be easier in the shower with soap or wash lotion, as the slick skin makes lumps easier to feel.
- Compare both breasts: Make sure you carefully examine both breasts and note any differences. Compare the texture, size and shape of both breasts.
- Watch for skin changes: Check for redness, dimpling or retraction that could indicate changes in breast tissue.
- Consider tissue consistency: Don't be alarmed if the tissue feels a little lumpy the first time you check — this is common, especially in younger women. Changes in consistency do not necessarily indicate cancer. When palpating, note whether the tissue moves freely or whether you can feel a lump in the breast or armpit.
- Seek advice if unsure: If you are uncertain whether you are performing the self-exam correctly or you discover changes, consult your gynaecologist for professional advice.
- Act immediately on changes: If during self-examination you detect lumps, changes in the breast or nipple area, inverted nipples, skin redness or unusual discharge, see a doctor promptly to investigate possible causes.
- Don't forget regular mammograms: While self-examination is important, it does not replace professional screening. These screenings are particularly important to detect early, non-palpable changes in breast tissue.
Breast cancer remains one of the major health challenges for women worldwide, but advances in early detection and treatment offer hope and opportunities. Through regular self-exams, targeted screening such as mammography and a healthy lifestyle, you can not only reduce risk but also, if necessary, significantly improve chances of cure.