Heel spur
Get rid of the pain with every step
How does a heel spur present?
The heel spur is a thorn-like bony outgrowth on the calcaneus (heel bone). Two main types are distinguished: the posterior heel spur, which occurs at the attachment of the Achilles tendon (cranial heel spur), and the plantar heel spur, which is more common on the sole of the foot (plantar heel spur).
The typical symptoms of a heel spur are varied. Affected people often feel a sharp, pinpoint pressure pain on the inner side of the foot near the heel bone. This can be perceived as burning, drilling or stabbing. Symptoms are usually worst in the morning on getting up and ease somewhat during the day.
After rest periods, pain increases on resuming activity, which is called start-up pain. Chronic tendon inflammation can lead to a continuous pain. With a posterior heel spur, the Achilles tendon insertion in the upper heel area may be swollen and red and painful to pressure.
What are possible causes of a heel spur?
A heel spur mainly develops from overuse of the foot, causing small injuries and tears at the insertion points of the plantar fascia or Achilles tendon on the heel bone. These micro-injuries can trigger inflammation, attracting immune cells to repair the tissue. Small calcifications form and eventually the heel spur appears.
Various factors increase the risk of developing a heel spur. Overweight puts greater pressure on the heel with every step, certain occupations require a lot of walking or standing, and genetic predisposition also plays a role.
Foot deformities such as high arches or pes planovalgus can, if untreated, promote the development of a heel spur. Poor footwear – too small, too tight, excessively high heels, thin soles or insufficient cushioning – also contributes to increased stress on the foot and thus to spur formation.
Insufficient warm-up before sports may leave muscles, tendons and ligaments more tense and thereby increase force on the tendon insertion at the heel. With increasing age, the fat pad under the heel shrinks, leaving tendons and bones less cushioned and more stressed.
How do orthotic insoles work against a heel spur?
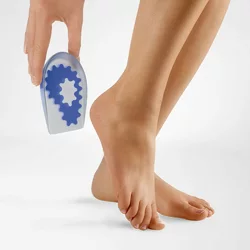
To relieve foot pain caused by a heel spur, special insoles are used. These are custom-made so that they contain a cut-out at the site of the thorn-like spur. The spur is thereby partially relieved and overloading avoided. This design protects the foot arch and reduces the pain caused by the heel spur.
In addition to insoles, there are various heel pads. These are placed in the shoes instead of the insoles and have a similar effect.
It is important to note that not every shoe is suitable for people with a heel spur. Many patients prefer shoes with particularly soft soles and insoles. Although insoles or specialised shoes can relieve pain, they do not remove the underlying cause of the spur, the calcification.
What helps with heel pain?
Treatment of heel pain, especially heel spurs, aims to relieve the tendons. This is achieved through temporary rest of the foot, supported by heel pads that reduce pressure on the heel and may allow the inflammation to subside. In the long term, insoles are often prescribed to support the foot in a targeted way.
In the acute inflammatory phase, analgesic and anti-inflammatory medications or ointments can help. Additionally, shockwave and ultrasound therapy may be used to reduce pain. Complementary physiotherapy may be prescribed to learn specific exercises that stretch and strengthen the muscles and tendons of the foot.
Surgery to treat a heel spur is performed only very rarely and as a last resort when other measures have failed. If necessary, part of the plantar fascia can be cut to relieve the tendons. However, this can lead to a flat foot, which is why surgery for heel spurs is an absolute exception.
Which doctor diagnoses and treats a heel spur?
The general practitioner or an orthopaedic specialist is primarily responsible for diagnosing and treating a heel spur. It is important to see these specialists, describe the symptoms and seek medical advice on treatment. For diagnosis, various procedures such as ultrasound, magnetic resonance imaging (MRI), video-assisted gait analysis or blood tests may be used for further clarification.
What helps prevent a heel spur: useful tips
- Wear comfortable shoes with a soft, well-fitting footbed.
- Choose suitable footwear and change it as often as possible. Worn-out shoes and those with a large heel-to-toe drop encourage the development of a heel spur.
- Monitor your weight. Overweight often means excessive pressure on the heel.
- Try to acclimatise gradually to barefoot walking. In doing so, weight is transmitted not primarily through the bone-joint chain but through the muscle-fascia chain. This is particularly suitable in summer when you can walk outside on different surfaces. Meadows, moss and sand are especially suitable.
- Mobilise and activate your foot muscles regularly.
- When playing indoor sports, wear specific indoor shoes with good cushioning.
- Sit down as often as possible, especially in occupations that require prolonged standing or walking.
- Stretch your calves regularly. Stand facing a wall with the affected foot forward and both knees bent. Move close enough to the wall so that the toes touch it. Lift the toes and bring the heel closer to the wall until only the heel touches the ground. Shift your weight forward until you feel a stretch in the calf, keeping the knee slightly bent. Hold the stretch for 30 seconds while breathing evenly. Recommended: 3 sets of 30 seconds each.
- Benefit in the long term from regular, independent training.
A heel spur can sometimes resolve on its own, but there is often a risk it becomes chronic and the pain persists. With targeted stretching exercises, physiotherapy treatments, appropriate footwear and offloading the foot with insoles, a heel spur can generally be well managed.