Papilloma
The often-overlooked signs of sexually transmitted infections
editorial.overview
What are human papillomaviruses (HPV)?
A papilloma is a benign overgrowth of skin or mucous membrane cells that can occur in different parts of the body. They are typically found on the skin, in the mouth lining, in the nose, in the urinary tract, in the milk ducts of the breast or in the larynx. Sometimes they are flat, sometimes elongated and stalk-like. Papillomas resemble warts and are therefore sometimes referred to as skin warts.
The causes of papilloma formation are often unclear. They can, however, be caused by human papillomaviruses (HPV). These are pathogens that can trigger inflammation and changes in the skin. These viruses enter through small cracks or injuries in the skin or mucosa and multiply within the cells.
Transmission of HPV occurs through direct contact with infected skin or mucosal areas. An HPV infection can cause different types of warts and increase the risk of cancer, particularly cervical cancer.
What symptoms occur with an HPV infection?
An infection with human papillomaviruses (HPV) usually runs without noticeable symptoms. Clinicians speak of a silent infection because the viruses settle unnoticed in the skin cells at the site of infection (e.g. in the genital, anal or oral and pharyngeal area), multiply there and may be transmitted to sexual partners. In most cases the viruses are sooner or later eliminated by the immune system. However, about ten percent of infections can become chronic.
A possible manifestation of an HPV infection is genital warts, which can develop as benign skin growths in the genital and anal area. These warts can vary in shape and have a whitish, reddish or grey-brown colour. They often appear in clusters and can merge into larger formations. Genital warts can disappear on their own, but persistent and troublesome warts should be removed.
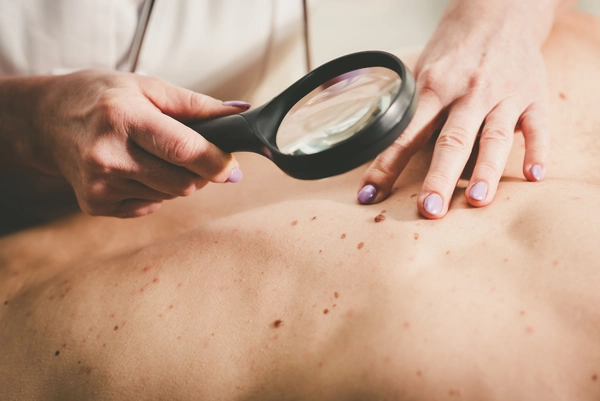
How do women detect an HPV infection?
Women can detect an HPV infection through regular screening, particularly with the Pap test. This identifies abnormally changed cells on the cervix that may indicate an HPV infection or a precursor to cervical cancer. If cellular changes are suspected, the patient is usually additionally tested for HPV.
The treatment for detected cellular changes or a precancerous stage of cervical cancer is to remove the affected tissue to prevent cancer from developing. With effective early detection and treatment, most cases of cervical cancer can be successfully prevented.
How do men notice an HPV infection?
Men often do not notice an HPV infection, as it usually causes no symptoms. In some cases, however, genital warts may occur in the genital and/or anal area. There is no official HPV test for men. Diagnosis is made through a medical examination. Genital warts can be treated by freezing, electric current or laser vaporisation. For larger areas, surgery may be required. General practitioners or urologists can help with HPV.
What conditions can HPV cause?
The different human papillomaviruses (HPV) have different effects on the body. Some infect primarily the skin, while others preferentially affect the mucous membranes. Common skin warts mainly occur on the face and on the hands and feet and are usually harmless. They are generally not caused by the HPV types that infect the genital area.
Benign genital warts, also called condylomas or anogenital warts, are mainly caused by about 40 HPV types that infect the genital organs and anus. The best-known low-risk types that cause these warts are HPV 6 and HPV 11.
Cellular changes in the anogenital area are another possible consequence of an HPV infection. In particular, high-risk types of HPV can trigger such changes. These may sometimes heal without treatment, but they can also lead to precancerous lesions from which cancer may develop in some cases.
Cervical cancer is the most common HPV-related cancer worldwide. HPV can also cause cancers of the vulva, vagina, penis, anus as well as of the mouth, throat and larynx.
How much protection does the HPV vaccine provide against cervical cancer?
The HPV vaccine does not provide complete protection against cervical cancer, but it is very effective in preventing HPV-related cancer. It protects against the HPV types most commonly causing cervical cancer and can also reduce the risk of genital warts.
The vaccine is particularly effective in adolescents before first sexual intercourse. It protects against high-grade dysplasias, the precursors of cervical cancer, and significantly reduces the risk of developing cervical cancer.
The vaccine is generally safe, with transient side effects such as pain at the injection site. Vaccine protection lasts for at least eight years, and the need for a booster dose is still unclear.
How to prevent HPV-related diseases: important tips
- Use condoms during sexual intercourse to reduce the risk of HPV transmission, even though they do not provide full protection.
- Maintain a healthy lifestyle, including a balanced diet and regular physical activity, to strengthen your immune system and reduce the risk of HPV infection.
- Consider vaccination as one of the safest protective measures against HPV infections. Note, however, that vaccination is not effective if an infection is already present.
- Take the opportunity to have girls and boys aged 9 to 14 vaccinated against HPV.
- Use the available vaccines that protect against high-risk types HPV 16, 18 and other types.
- Observe good hygiene practices, especially in the genital area, to minimise the risk of HPV infection.
- Avoid direct contact with warts, especially if you have close contact with people who have HPV warts.
- Do not share towels or clothing with people who have warts to prevent possible transmission.
- Wear (bath) shoes in public areas such as hotel rooms, saunas or public baths to reduce the risk of infection from direct contact with contaminated surfaces.
HPV infections can occur in both women and men and often proceed without noticeable symptoms. There are different HPV types that can have varying effects on the body, including the formation of warts or precancerous lesions. Vaccination, healthy lifestyle habits and hygiene measures are important protective measures.