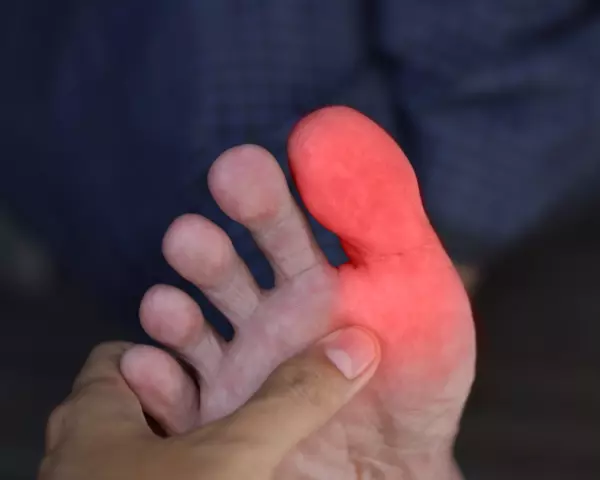
Osteoarthritis
Movement helps against this disease
editorial.overview
What is osteoarthritis?
Osteoarthritis is a degenerative joint disease in which the cartilage layer between joint surfaces is gradually worn away. The cartilage, which normally acts as a shock absorber and allows smooth joint movement, becomes thinner and less elastic over time. This can lead to pain, stiffness and reduced mobility.
In advanced cases, joint stiffening may even occur, which can significantly limit freedom of movement. Osteoarthritis can affect different joints and, in some cases, several at the same time — this is referred to as polyarthrosis. The condition occurs to varying degrees and can greatly affect quality of life.
What causes osteoarthritis?
Osteoarthritis usually develops from mechanical overload of the joint cartilage, where destructive processes exceed the cartilage's natural regenerative capacity. This overload can have several causes.
Frequent or intensive physical strain, whether due to occupational activities or sports, can heavily stress the joint cartilage. Occupations that involve heavy loads or repetitive movements, such as construction workers or professional athletes, are particularly prone to premature cartilage wear.
Joint malalignment or damage to ligaments and soft tissues can lead to uneven loading of the cartilage. This abnormal load accelerates cartilage breakdown and can contribute to osteoarthritis development. Previous injuries, such as fractures or sprains, can also have long-term effects on joint health.
Joint infections, particularly bacterial ones, can cause inflammation and damage cartilage. Inflammatory rheumatic diseases, such as rheumatoid arthritis, can also lead to secondary osteoarthritis, where the joints are significantly damaged by the inflammatory condition.
The likelihood of developing osteoarthritis increases with age, as cartilage naturally loses elasticity and resilience over the years. Up to the age of 55, men are more frequently affected, whereas the disease is more common in women at older ages. Genetic factors also play a role, especially in osteoarthritis of the finger joints, where a family predisposition can increase the risk.
Osteoarthritis is therefore influenced by a variety of factors, from mechanical overload and malalignment to genetic and inflammatory causes. Understanding these causes is crucial for taking preventive measures and developing targeted treatments.
How does a healthy joint work and when does osteoarthritis start?
A joint functions as a finely tuned system of articular cartilage, bone, ligaments and synovial fluid. The cartilage that covers the joint contact surfaces acts as a shock absorber and ensures smooth, pain-free movement. It contains no nerve endings, which is why cartilage damage is often noticed only when it reaches the underlying bone. That bone, particularly the pain-sensitive periosteum, reacts to pressure and movement with severe pain.
Osteoarthritis begins when the natural balance between cartilage-degrading and -regenerating processes in the body is disturbed. With increasing age, the cartilage's ability to retain water decreases — a property essential to its elasticity and strength. The cartilage becomes thinner, more fissured and loses its sliding properties, making joint surfaces rougher and less smooth. These changes increase friction and ultimately cause further cartilage loss.
When cartilage is completely worn away, bone fragments can be released, worsening symptoms. In advanced stages of osteoarthritis an inflammatory reaction may occur. The joint swells, feels warm and becomes very painful — this is called activated osteoarthritis. Pro-inflammatory mediators accelerate further cartilage breakdown, perpetuating the cycle of damage and inflammation.
Which tissues can be affected by osteoarthritis?
Osteoarthritis affects not only the articular cartilage but can involve various other tissues within and around the joint. As osteoarthritis progresses, cartilage is increasingly degraded, placing stress on the underlying bone structure. This can lead to bone growths at the margins of the joint surfaces, known as osteophytes. The bone beneath the most heavily loaded cartilage layer can also thicken, a change known as subchondral sclerosis. In heavily loaded areas bone cysts may form and be visible on X-rays.
Inflammatory processes during osteoarthritis damage the ligaments and tendons that stabilise the joint. These injuries lead to reduced stability and function of the joint. Protective posture often leads to wasting of the surrounding muscles, which worsens the situation.
The joint capsule can also be affected by the disease. Inflammation of the capsule may cause thickening and hardening, which further damage the joint and limit mobility.
In summary, osteoarthritis influences the entire joint structure. Progressive cartilage loss and related changes in adjacent bones, ligaments and tendons can lead to deformities, painful movement and ultimately complete joint stiffening. This process can indirectly damage neighbouring or contralateral joints, resulting in so-called secondary osteoarthritis.
What are typical osteoarthritis symptoms?
Typical osteoarthritis symptoms can be varied and troublesome. Pain often starts as a pulling or tension sensation on the first movement, especially after a period of rest, such as getting up in the morning or after prolonged sitting. Many people experience morning stiffness, where the joint is particularly stiff and difficult to move after getting up. This stiffness may improve during the day.
Pain often occurs during or after physical activity, for example after long walks or standing for extended periods. Initially it may be temporary but can become chronic over time. With an inflammatory reaction there may be joint swelling and warmth, often accompanied by an effusion. In advanced stages the pain can become constant and occur at night, significantly affecting quality of life.
The muscles around the painful joint may feel tense, adding to the discomfort. Joint mobility can be restricted, making daily activities more difficult.
These symptoms are important indicators of possible osteoarthritis and should be evaluated early by an orthopaedic specialist to confirm the diagnosis and initiate appropriate treatment steps.
Which joints are affected by osteoarthritis?
Osteoarthritis can occur in almost any joint of the body, with severity and symptoms depending on the tissue involved. According to studies by the Robert Koch Institute, the knee and hip joints are most commonly affected. More than half of patients with osteoarthritis report complaints in the knee joint, followed by about a quarter who suffer hip osteoarthritis. The finger joints are also frequently affected, particularly in women, while finger osteoarthritis is less common in men.
In addition to commonly affected joints such as the knee, hip and fingers, osteoarthritis can also damage the spine, shoulder, ankle and midfoot joints. The facet joints of the spine can rub painfully in facet joint osteoarthritis, while spondylosis involves wear of the intervertebral discs and vertebral bodies with bone spurs. Shoulder osteoarthritis is less common but occurs more often in older people. In the ankle and midfoot, osteoarthritis can appear in younger patients, especially after sports injuries or without an obvious cause.
How does the doctor diagnose the disease?
To diagnose osteoarthritis, the doctor first takes a comprehensive medical history, during which the patient describes their complaints. A thorough clinical examination follows, in which the doctor examines the affected joint for swelling, pain and movement restrictions. Laboratory tests are usually unremarkable, as osteoarthritis does not produce specific lab markers.
Imaging techniques play a central role in diagnosis. Joint ultrasound and X-rays are particularly important. Joint ultrasound can help visualise soft tissue changes and fluid accumulation in the joint, while the X-ray shows typical signs of osteoarthritis such as cartilage loss, bone growths or narrowing of the joint space. An arthroscopy is usually considered only if the doctor needs additional therapeutic measures or suspects a specific finding such as a meniscal injury.
What helps with osteoarthritis?
Treatment for osteoarthritis aims to preserve remaining cartilage and relieve pain, since destroyed cartilage cannot be regenerated. In early stages of the disease, exercise is essential. With severe pain, treatment focuses on controlling symptoms. Treatment options include non-drug measures, pharmacological treatments and, if necessary, surgical interventions.
In early stages, osteoarthritis can often be managed without medication. Non-drug approaches include physiotherapy, physical therapies, maintaining a normal body weight, avoiding smoking and excessive alcohol consumption, and assistive devices such as braces or walking sticks.
Pharmacological therapies mainly include non-steroidal anti-inflammatory drugs (NSAIDs), which can relieve pain and inflammation but do not cure osteoarthritis and may cause side effects. In advanced osteoarthritis with severe pain, cortisone injections can help reduce joint inflammation. In very severe cases, surgical procedures may be required, such as joint-preserving operations, joint replacements or, in some cases, arthrodesis to minimise pain and improve quality of life.
Effectively preventing osteoarthritis and supporting treatment: helpful tips
- Integrate targeted exercises into your daily routine to keep joints flexible. Activities such as swimming, cycling and Nordic walking are particularly joint-friendly and effective. Avoid sudden, jerky movements that may overload the joints.
- Prefer moderate endurance exercise over high-performance sports to spare your joints and strengthen the muscles around them. Aqua jogging and water gymnastics are also recommended. Avoid extreme sports that place heavy stress on the joints.
- Have congenital or acquired misalignments treated promptly to prevent overload and damage. Orthotic insoles or surgical corrections can be helpful.
- Pay attention to correct movement patterns in daily life and at work. Avoid one-sided strain and correct non-physiological movements.
- Follow a balanced diet with plenty of fresh vegetables, fruit, high-quality vegetable oils and oily fish. Reduce consumption of meat, sugar and highly processed foods to minimise inflammation.
- Maintain a healthy body weight to avoid additional stress on the joints. Overweight can accelerate joint wear and increase pain.
- Avoid heavy manual labour and knee-straining activities. Use aids such as walking aids or braces if necessary to relieve the joints.
- Try alternative methods such as cooling compresses with quark, cabbage or healing clay for pain relief. Herbal preparations like devil's claw and arnica extracts may also provide support, but should be discussed with a doctor.
- Use cold therapy for inflamed joints to reduce swelling and pain. Heat can be soothing for muscle tension around the joint.
- Reduce stress, as it can amplify pain and negatively affect joint health. Relaxation techniques and regular recovery periods are important.
- Have your joints checked regularly by an orthopaedic specialist. With progressive osteoarthritis, early diagnosis and treatment can be important to slow the course of the disease.
Osteoarthritis is a complex interplay of biological and mechanical factors that can significantly affect daily life. Through preventive measures, targeted exercise and a healthy lifestyle, however, the progression of osteoarthritis can be slowed and quality of life improved.
.png.webp)