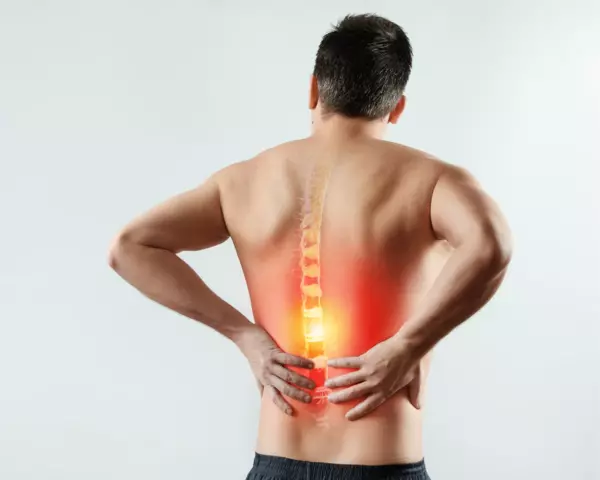
Pain therapy
These are the ways out of hell
editorial.overview
What exactly is pain therapy?
Pain therapy includes all treatment measures that help to relieve pain and improve the quality of life for those affected. It is primarily aimed at people with chronic pain that significantly interferes with daily life.
The goal of pain therapy is not necessarily complete freedom from pain, but a tolerable state that allows patients to regain more enjoyment in life. In addition to medications, therapy focuses on strategies that encourage greater social, physical and cultural activity. Acute pain is treated to prevent chronification, while chronic pain is approached holistically.
What is the difference between acute and chronic pain?
Acute and chronic pain differ mainly in their duration, cause and function.
Acute pain occurs suddenly and has a clear protective function: it warns of injury or overload and triggers reflexes such as quickly withdrawing when touching a hot surface. These pains are caused by tissue damage and the pain signal is transmitted almost instantly to the brain via specialised nerve pathways. The body reacts, sometimes with temporary pain relief from naturally produced endorphins.
Chronic pain, on the other hand, persists for more than six months, often independently of direct tissue damage. Chronic pain arises from changes in the nervous system, leading to a so-called "pain memory". Even minimal stimuli can trigger pain in this way, even without an acute cause. Chronic pain has no protective function and affects life in the long term, often accompanied by sleep disturbances, fatigue and reduced mobility. Examples include conditions such as rheumatism, osteoarthritis or fibromyalgia.
What treatments are available for chronic pain?
Chronic pain can significantly restrict everyday life and often leads to considerable burden. To prevent the development of chronic pain or to alleviate existing symptoms, specialised and early pain therapy is crucial.
The so-called multimodal pain therapy, which has proven effective particularly for long-lasting or recurring pain, combines different treatment approaches. Medicinal, physiotherapeutic and psychological measures and sometimes invasive procedures are coordinated and used together. The aim is to treat pain as a whole, improve quality of life and have a lasting influence on the body's pain memory.
How does multimodal pain therapy work?
Multimodal pain therapy is an integrative approach designed to reduce chronic pain and its impact on daily life. It is usually carried out by an interdisciplinary team of doctors, psychologists and therapists who draw up an individual treatment plan after comprehensive diagnostics.
The process begins with a thorough assessment that takes into account not only the patient's medical condition but also psychological and social aspects of pain. An important part of therapy is patient education. Patients learn about how their body works, the causes of pain and how they can better understand and manage their symptoms.
Therapy includes both individual and group sessions with different focuses. Physical activation through physiotherapy and exercise therapy plays a central role, with targeted exercises to strengthen and stretch muscles. Joy of movement is rekindled and patients learn techniques to overcome fear of movement and pain.
Psychological support is also an essential part of multimodal pain therapy. Chronic pain is often influenced by stress, anxiety and negative thoughts. Psychological pain therapy aims to identify these psychological burdens and reduce them using targeted techniques such as stress management, mindfulness and cognitive restructuring. This helps patients cope better with pain and improve their quality of life.
Relaxation techniques and methods for regulating tension are also introduced to help patients release tension and improve body awareness. The knowledge and techniques learned should then be integrated into daily life to promote self-management of pain and enhance quality of life in the long term.
Occupational therapy and nutritional counselling complement the treatment plan to increase physical and mental resilience and promote a healthy lifestyle. In some cases, alternative therapies such as acupuncture, neural therapy or homeopathy are considered to provide additional relief.
The aim of multimodal pain therapy is to enable patients to manage their chronic pain autonomously, regain zest for life and prevent the chronification of pain. Progress is regularly reviewed throughout the process and adjustments can be made to the therapy to achieve the best possible outcomes.
What are the benefits of heat in pain treatment?
Heat therapy offers a variety of benefits in pain management. It uses different heat sources such as hot air, infrared or warm packs with peloids to warm tissues and stimulate circulation. This promotes the removal of metabolic waste products and inflammatory substances and supplies affected areas with more oxygen and nutrients.
Deep heat in particular, which reaches deep muscle layers, relieves tension and promotes relaxation of the tissues. Locally applied, heat also stimulates thermoreceptors, resulting in fewer pain signals reaching the brain – this reduces pain intensity. Vasodilation and the stimulated metabolism support tissue repair.
Heat therapy is particularly effective for non-inflammatory pain and chronic pain conditions caused by muscle tension or circulatory disorders. Common indications include osteoarthritis and rheumatic diseases, back and neck pain, muscle tension, menstrual pain and fibromyalgia. However, heat therapy is not suitable for acute inflammations, as heat can worsen symptoms in those cases.
What is the goal of psychological pain therapy?
The goal of psychological pain therapy is to break the cycle of pain, anxiety and depression that often severely impairs the quality of life of people with chronic pain. Psychological care is therefore an essential component of pain therapy.
Using behavioural measures such as cognitive therapy, attention training, self-care and relaxation exercises (e.g. progressive muscle relaxation and autogenic training), patients are helped to recognise and change the connection between their mental states and pain perception. Modern imaging techniques make it possible to visualise the links between somatic pain perception and emotional processes in the brain. These insights help to understand how emotions such as sadness, anxiety or helplessness can intensify the perception of pain.
A central aim of psychological pain therapy is to identify and change unhelpful behaviour patterns that can contribute to the persistence of pain. By strengthening self-acceptance, self-efficacy and self-esteem, therapy promotes an optimistic-yet-realistic mindset and supports patients in better accepting and coping with their pain.
Overall, psychological pain therapy aims to reduce the negative effects of chronic pain and improve the quality of life of those affected by fostering a better understanding of their own physical and psychological processes.
What to do for chronic pain: tips to improve quality of life
- Regular physical activity is crucial. Activities such as hiking, brisk walking, swimming and cycling can have a positive effect on pain perception. Start slowly and gradually increase intensity to avoid overload.
- Work with a physiotherapist to introduce light equipment-based training into your daily routine. This can help strengthen and stretch muscles and relieve pain.
- Use massages, heat and cold applications as well as electrotherapy (TENS). These methods can release muscle tension, improve circulation and reduce pain.
- Try acupuncture. This traditional Chinese medical method can be helpful for certain types of pain such as headaches, rheumatism and osteoarthritis. Check whether this treatment is covered by your health insurance.
- Learn relaxation techniques. Methods such as progressive muscle relaxation or autogenic training can help reduce stress and decrease pain perception.
- Pain coping strategies based on cognitive behavioural therapy can help you identify and change negative thought patterns associated with your pain.
- Join self-help groups. Exchanging experiences with others affected can provide emotional support and open up new perspectives on living with chronic pain.
- Consider functional training. Your doctor can prescribe functional training for up to 24 months to specifically work on improving mobility and pain management.
- A balanced diet can support overall health and reduce inflammation in the body, which can positively affect pain relief.
- Discuss your pain and progress regularly with your doctor or pain therapist. Alternative therapies or adjustments to your treatment plan may be possible to achieve better symptom relief.
Pain therapy is more than just pain relief – it is a holistic approach that considers body, mind and social environment. Through individually tailored treatment strategies ranging from medication to psychological to physical methods, people can learn to live with their pain and improve their quality of life. With the right support it is possible not only to regain control over pain but also to lead a fulfilling life despite the challenges pain may bring!